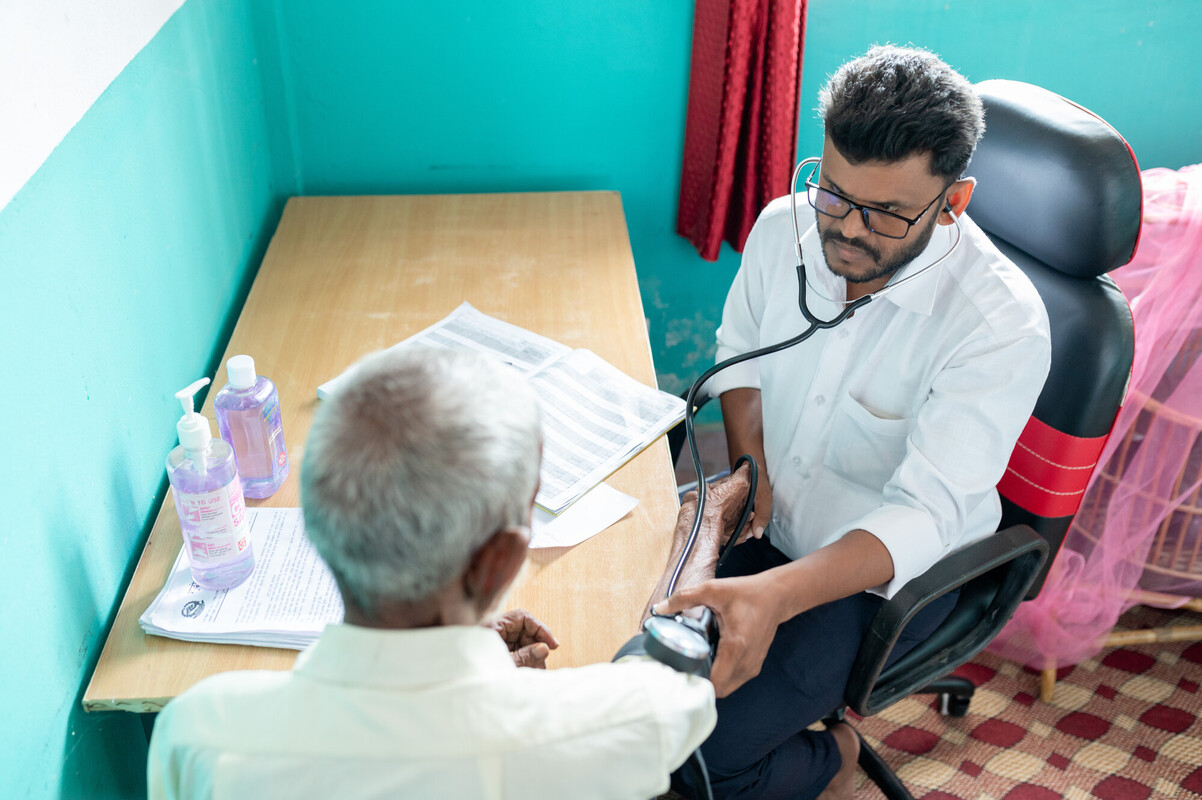
Scientific breakthroughs, from simplified antiretroviral therapy to long-acting prevention technologies, have put HIV epidemic control within reach. Nevertheless, as any long-distance runner will assert, the last mile inevitably proves to be the most challenging. After four decades of remarkable progress, what has brought us to the brink of achieving the UNAIDS 95-95-95 targets is likely insufficient to accelerate and sustain progress across the finish line.
As the world observes World AIDS Day 2025, the global HIV community stands at a pivotal moment. This year’s theme: Rethink, Rebuild, Rise, reflects both the progress made and the urgency that remains. It calls for renewed local leadership, innovation, solidarity and resilience as the global community works together toward an AIDS-free generation.
Rethink: Redefining support as local actors lead the HIV response
Across the world, local actors and governments are assuming greater responsibility for financing, managing and delivering HIV programs. Scientific advances such as the World Health Organization’s 2025 recommendation of long-acting injectable lenacapavir (LEN) signal a new era in HIV prevention. Yet the real test lies in ensuring that these innovations are integrated, scaled, and sustained within national systems.
Global partners must support governments to maximize the impact of the domestic investments they mobilize, ensuring plans close rather than create access gaps, optimize medicine and commodity allocation and use, and maintain high-quality services with the flexibility to adapt. Many countries are already buying their own medications but have critical challenges ensuring that these commodities are available in the right places, at the right time, and before they expire. In addition, even when commodities are available, clients face enormous social and economic barriers to initial and continued access that can only be overcome with investments to address those barriers. As global partners continue to follow local leadership, we must tailor our support to each country’s national plan, helping governments to optimize the impact of their expanding domestic investments.
Rebuild: Strengthening systems for sustainability
As game changing as LEN promises to be, biomedical advances alone cannot transform the epidemic without strong and adaptable systems that ensure access, quality and continuity of care.
Health systems must be capable of delivering high-quality HIV services, retaining people in treatment, achieving viral suppression and preventing new infections – including the elimination of mother-to-child transmission (eMTCT). These goals require structural investments in data, supply chains, workforce and financing that extend beyond any single intervention.
Rwanda offers one of the clearest examples of how strong systems can drive sustained HIV progress. The country is widely recognized for its effective health governance, long-term national planning and fully institutionalized community health workforce. Rwanda’s data-driven systems, including national dashboards – used to track viral suppression, treatment continuity, and maternal outcomes – underpin its integrated approach to HIV, maternal, newborn and child health, as well as eMTCT. Its national adoption of multi-month dispensing of medication, differentiated service delivery, supply chain reform and partnerships with the private sector demonstrate sustainable, scalable models.
Strong health systems ensure that countries can manage the evolving HIV landscape while integrating innovations efficiently and sustainably. They are the foundation for true self-reliance and epidemic control.
Rise: Advancing community leadership and access for all
Despite unprecedented progress, stigma, discrimination and social exclusion continue to limit access to lifesaving services. Governments across the world have articulated a shared ambition to provide access to HIV services, because epidemic control cannot be achieved without it. Realizing this ambition requires systems that respect the need of every individual, amplify community voices and dismantle barriers to care.
To advance this vision, the global community must partner with community-led and grassroots organizations – including networks of people living with HIV, people vulnerable to contracting HIV, and faith-based groups – to co-design, implement and monitor HIV prevention and treatment programs that reflect lived realities and local priorities. Thailand’s experience with community-led, community–focused services, demonstrates how inclusive programming accelerates progress toward epidemic control where conventional facility-based approaches have plateaued. Through the community-led model, where peer navigators, community clinics and lay providers deliver HIV testing, PrEP, antiretroviral therapy initiation and retention support, the country has achieved some of the highest viral suppression rates among at-risk populations. These gains were only possible because the programs were designed and delivered by the communities most affected, breaking down stigma, increasing trust and expanding access in ways traditional health facilities could not. Thailand’s success shows that when communities lead, barriers fall, uptake increases and epidemic control becomes achievable, while programs that fail to include most affected groups continue to see stagnation and widening gaps.
A shared commitment to the future
If countries, communities and partners work together, we can achieve an AIDS-free generation. The path forward requires global solidarity, national leadership and enduring commitment.
At FHI 360, this commitment is reflected in every facet of our work, from developing global guidance and operational research to providing tailored technical support that strengthens national programs. Our mission is clear: to ensure that science serves people, that every breakthrough reaches those who need it most, and that the promise of an AIDS-free generation becomes a shared reality for all.