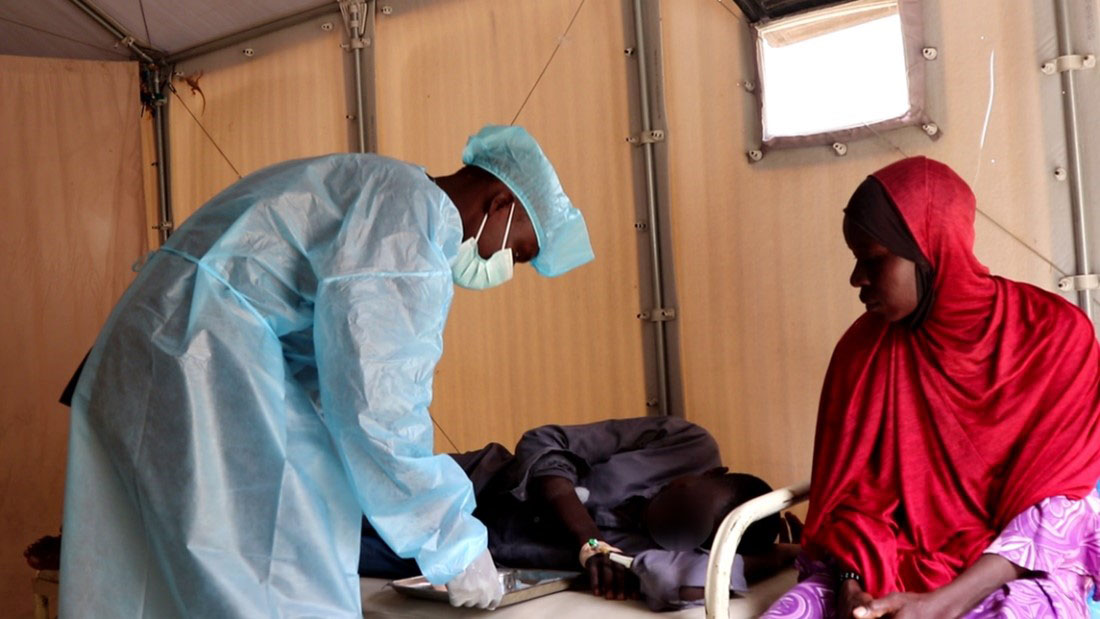
By 8 a.m., as many as a dozen patients were already waiting to see a doctor at FHI 360’s cholera treatment unit in Borno State, Nigeria. In September 2022, the country was hit by its worst cholera outbreak since 2017. With the upcoming rainy season, which has worsened over time due to global climate change, doctors must again prepare to treat patients.
Last year’s cholera outbreak was exacerbated by factors such as dangerous floods and large-scale displacement. The result: an unusually high volume of patients.
If untreated, cholera can become fatal in just hours. The diarrheal disease is caused by ingesting contaminated food or water, and areas with inadequate water, sanitation and hygiene services are especially prone to outbreaks. There are about 1.3 billion people worldwide who are at risk of contracting cholera in countries where local transmission occurs, according to the U.S. Centers for Disease Control and Prevention.
To help address the transmission in Nigeria’s Borno State, FHI 360’s crisis response team operates cholera treatment units in three different towns and supports a government-operated cholera treatment unit.
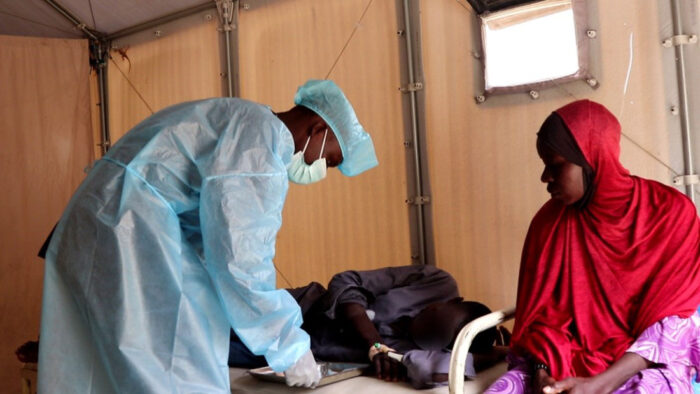
Centers running low on supplies
“We basically have a whole lot to do as early as we are allowed to be at the [cholera treatment unit],” says Dr. John Paul Ezeokeke, technical officer of health and nutrition at FHI 360. But there have been challenges, such as difficulties with transporting patients to the treatment units, supply shortages and insufficient numbers of staff.
“You cannot plan for the total number of patients that you will see at the beginning of your preparation,” says Dr. Ngita Bwala Siki, technical officer of health and nutrition at FHI 360. “The patient turnout [last year] was far more than stocks we [had] available to attend to those patients. So, at some point, we had rapid depletion of our stocks in terms of fluids, [oral rehydration solutions] and other medications.”
The team created an emergency plan to transport stock from Maiduguri (the capital of Borno State), and partners sent supplies and staff. Eventually, the team secured enough help to handle the number of patients coming in.
Samuel Nehri, a laboratory scientist at FHI 360 who works with Siki at the same treatment unit, says that the team treated more than 1,000 patients in their unit in less than six weeks. The unit has 60 beds.
Preparing for future cholera outbreaks
With the upcoming rainy season, medical personnel must again prepare for the worst. Generally lasting from May to October in the Borno, Adamawa and Yobe States, the period is characterized by heavy rainfall and flooding, which can lead to contaminated water sources and an increased risk of water-related and fecal-oral diseases, such as cholera. Many experts also believe the effects of climate change contribute to cholera outbreaks.
Displacement is a frequent risk factor of cholera, as people who are displaced often live in close quarters and lack reliable access to water, sanitation and hygiene services. Last year’s outbreak was no exception. Near one of the treatment units, there are four camps for people who are displaced. After some camps in Maiduguri closed, many displaced people sought shelter at those four camps. The first cholera case was reported among these people.
The effect of the outbreak on medical personnel
Treating the cholera outbreak has required sacrifices from medical, hygiene and logistics professionals and has taken a toll on the surrounding community.
“We are basically taking a lot of risks,” says Ezeokeke. He explained that health workers serving people in hard-to-reach local government areas were often in the center for long hours due to high caseload.
Dr. Andrew Okwoli, field coordinator at FHI 360 who works with Ezeokeke at the same treatment unit, says it was difficult to sit down even for a 15-minute break. “You have some patients coming in who are critically ill, and you just have to keep pushing to ensure that they are provided the required care.”
But there were moments of beauty during last year’s outbreak, too. Ezeokeke recalled a woman who went into labor a day into her admission and gave birth at the unit. “That went a long way to put smiles on our faces, and very much encouraged us to do more,” he says.
Containing a cholera outbreak
While FHI 360’s medical staff worked to save the lives of patients, our field teams worked with partners to contain the outbreak in communities outside the treatment units.
“It was basically an all-hands-on-deck approach that we applied while also ensuring that, at the community level, a whole lot of sanitization [activities], active case finding and other components of our primary prevention [strategy] were put in place,” says Ezeokeke.
When working to contain a cholera outbreak, it is important to identify the source of contamination, promote hygiene awareness and provide a safe water supply. But according to Julia Rosenbaum, technical advisor with FHI 360’s water, sanitation and hygiene team, “the long-term prevention of cholera lies in economic development and universal access to safe water and adequate sanitization.”

A community volunteer uses chlorine solution to disinfect the floor of a cholera treatment unit run by FHI 360 in Borno State, Nigeria. Photo credit: Ayodeji Daniel Adeyemo/FHI 360
Cholera has existed for centuries. Its causes are complex, and the effects of climate change are only making them more so — with more flooding, more displacement of people and greater challenges to providing adequate sanitation and hygiene services. Mobilizing quickly, as FHI 360 has done in Nigeria, to support communities during crises is key to minimizing the impact of cholera and containing future outbreaks.